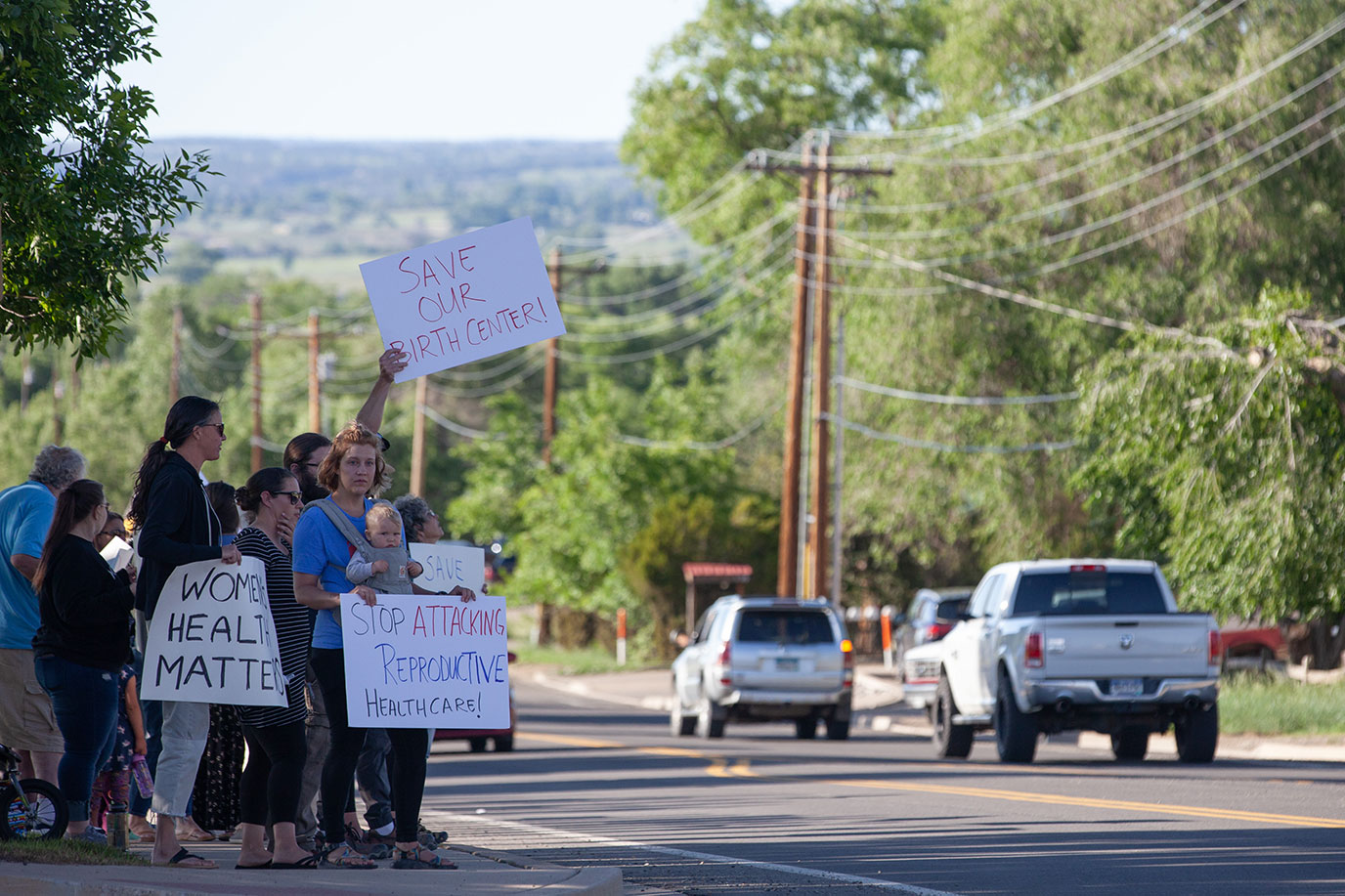When a woman arrived to give birth at Southwest Memorial Hospital in Cortez, Colo., on a Monday evening in early June, she went into labor and Erin Schmitt, DO, the attending OB-GYN, helped deliver her baby within 15 minutes—about as straightforward a birth as Schmitt was likely to see. But an hour later, a nurse called Schmitt to say the woman was bleeding. Soon after, Schmitt was dealing with one of the most massive hemorrhages she had ever seen in her 10 years as a physician.
At 2 a.m. the next morning, Schmitt and an ICU nurse wheeled the woman back into the operating room. By the time Schmitt inserted a device called a Bakri balloon into the woman’s uterus to stop the bleeding, she had lost three liters of blood, but the device saved her life.
Schmitt has seen enough in her career to know that such birthing-related complications are surprisingly routine. Babies get stuck in the birth canal. Umbilical cords wrap around the baby’s neck. A woman hemorrhages.
“Luckily, the majority of them do just fine, but when they don’t you have to be able to react quickly,” Schmitt said. “If [the birth] hadn’t been here at the hospital, she wouldn’t have survived.”
More troubling, however, was where Schmitt found herself a week later: delivering this anecdote about that traumatic night to the Southwest Health System’s board of directors in a desperate plea to save the hospital’s birthing center, where Schmitt works.
In early June, Southwest Health System, the nonprofit that runs the hospital, announced it would temporarily close the birthing center on July 1, 2023, “based on financial and staffing needs,” according to a press release. Following a community-wide outcry over the closure, Southwest Health System reversed its decision 12 days later. The birthing center would remain open—at least for now, but for Schmitt and others invested in maternal health care, the fight to save the birthing center has just begun.
* * *
Originally from Massachusetts, Schmitt moved from New England to Shiprock, N.M. in 2013 to work at Northern Navajo Medical Center, which is run by the Indian Health Service and serves enrolled members of the Navajo Nation. A former Peace Corps volunteer, Schmitt was attracted to working with underserved and marginalized populations, which she felt added a lot of depth and interest to medicine.
Four years later, she was pregnant and looking to relocate to Cortez, a town of just under 9,000 in the southwest corner of Colorado. It’s a rural community, surrounded by mountains and high desert, and Schmitt was surprised to learn it had fewer health care resources than the Navajo communities served by the federally funded Indian Health Service.
At the time, Southwest Memorial Hospital had no gynecology services and no established obstetrics program. The few family physicians who practiced obstetrics were often overwhelmed with the need for prenatal care and deliveries.
“I found that the need was actually greater here in this rural Colorado area than it was in Shiprock, on the Navajo reservation,” Schmitt said.

Erin Schmitt, DO, an OB-GYN physician at Southwest Memorial Hospital in Cortez. Photo by Corey Robinson / Special to The Colorado Trust
Around the time that Schmitt and her husband were looking to move to Cortez, Southwest Memorial Hospital was looking to hire an OB-GYN with a surgical background to deal with the increasing number of high-risk labor and delivery cases like ectopic pregnancies and other complications. Schmitt was excited about the opportunity to make a difference in her adopted community and was hired in 2017.
According to Schmitt, her hiring was part of a big effort to improve the quality of care at Southwest Memorial, increase the services it provided, and gain the community’s trust. Along with Schmitt, the hospital hired a pediatrician, a pulmonologist, and two more general surgeons. The following spring, the hospital finished major renovations and opened a new building housing the labor and delivery unit. To help Schmitt, the hospital hired another OB-GYN, Jessica Kaplan, MD, in 2021.
Within a few years, Schmitt and Kaplan were averaging roughly 160 newborn deliveries annually and had doubled the number of hysterectomy surgeries (total removal of the uterus) from 14 to 28 per year. Schmitt was proud of what she and Kaplan were accomplishing in the birthing center.
But under the surface, the hospital was in deep financial trouble.
In 2018, a financial crisis nearly led to the hospital being closed, which resulted in Southwest’s board hiring Community Hospital Consulting, the management and consulting arm of Community Hospital Corporation, based out of Plano, Texas, to get the hospital’s finances under control. Forty staff were laid off, among other changes, and the hospital’s financial situation improved. As reported by The Journal, the Cortez newspaper, in 2020 and 2021 Southwest broke even and showed small profits.
When Kaplan arrived, she and Schmitt worked with two other physicians who did obstetrics in the birthing center, but with both nearing retirement, Kaplan and Schmitt began asking the hospital to hire another OB-GYN. They met with the interim practice administrator and the then-CEO of Southwest to ask about their plan for replacing the outgoing physicians.
“There was no recruitment plan,” Kaplan recalled. Instead, the hospital ended up relying on a locum physician—a contracted physician brought in from elsewhere—to be on call in the event of a labor, in accordance with regulations that mandate 24-hour OB-GYN coverage at a labor and delivery unit. (Southwest Hospital System did not agree to an interview, but in a written statement, Joe Theine, who was appointed Southwest Health System CEO over the summer, said that “recruiting healthcare professionals remains an important part of our work to help prepare for our future healthcare delivery needs.”)
Over time, Schmitt and Kaplan noticed other things, too. Many of the nurses who had worked at the hospital the longest—some upwards of 20 years—were leaving, with several saying it was due to frustrations with management. Services like optometry, pulmonology, and the pain and spine clinic were cut. (Southwest Hospital System declined to confirm exactly which services were eliminated or when.) To the two physicians, it seemed like Community Hospital Corporation was so hyper-focused on the bottom line that it didn’t prioritize the needs of the medical providers or those of the local community.
Meanwhile, the hospital was underwater again financially, exacerbated by the end of federal COVID-19 funding. In a June 7, 2023 recording of an employee forum obtained by The Journal, former Southwest Health System Interim CEO David Faulkner told employees that the nonprofit was in the red.
“We continue to lose money. So far this year to date, $1.4 million. We cannot continue on this track, and labor and delivery is a service that we lose significant money on,” Faulkner was quoted as saying.

Cortez community members gathered for a public meeting and questioned executives from Community Hospital Corporation, the company that manages Southwest Memorial Hospital in Cortez, during a hospital board meeting on June 15, 2023. Photo by Corey Robinson / Special to The Colorado Trust
* * *
Across the country, rural hospitals like Southwest Memorial are struggling under crushing economic realities. According to data from Chartis, a health care consulting firm, 43% of rural hospitals are operating with negative margins.
To cut costs, many have eliminated services, most notably chemotherapy and obstetrics, leaving communities across rural America without access to crucial health care. In these so-called “maternity care deserts,” pregnant people and infants must travel farther for prenatal and postnatal care, increasing the risk to parents and babies in the case of an emergency.
In Colorado, no rural hospitals have closed in recent years, in large part due to Medicaid coverage expansion and reimbursement rate increases, through both the 2009 state hospital provider fee law and the 2010 federal Patient Protection and Affordable Care Act. However, to remain financially viable, many have been forced to reduce services or partner with a larger multihospital system, either through purchase or an affiliation agreement. (The Durango hospital has for years been operated by Centura Health, now known as CommonSpirit.)
Obstetrics is often the first service to go since it’s the second most expensive department after the emergency room, said Michael Topchik, the national leader for the Chartis Center for Rural Health.
“Rural hospitals have such a small volume of births,” he said, noting that the majority of those births are reimbursed by Medicaid, which generally provides lower reimbursement rates—around $6,500 per birth—than private insurance companies, which offers about $15,000 per delivery.
According to Topchik, it’s not uncommon for hospitals operating under thin margins to hire management companies that promise to help turn things around.
“The bottom line is that providing [obstetrics] services is challenging,” Topchik said. “These rural hospitals are doing their darnedest to stay open. And sometimes, staying open means shuttering services that the community needs.”
Still, the results of such financial “optimizations,” as Topchik called them, can be uneven. When Sara Pikaart, a labor and delivery nurse who worked at the hospital operated by Rehoboth McKinley Christian Healthcare Services in Gallup, N.M., heard about Southwest’s troubles, she felt compelled to write a letter to the Southwest hospital board and warn them about what had happened to Rehoboth under Community Hospital Corporation management.
Like at Southwest in Cortez, Community Hospital Corporation took over management of Rehoboth McKinley Christian Hospital in 2020 because of the hospital’s financial difficulties. Afterward, “things quickly got worse,” Pikaart wrote. The hospital closed the labor and delivery department in 2022. Physicians and nurses went unpaid and left in response to unsafe staffing and mistreatment by the administration, Pikaart claimed; others were fired. (Rehoboth McKinley did not respond to multiple requests for comment.)
“Our department was run into the ground and eventually closed, leaving patients with limited and expensive options for care,” Pikaart said in her statement. Publicly, she added, the (now former) Rehoboth CEO blamed the nursing staff for the closure after they were forced out, claiming they had left for more lucrative travel assignments. (Pikaart says that every single member of the permanent nursing staff in her old department still lives in Gallup.)
Since Rehoboth closed its birthing center, other services followed—including outpatient women’s health, behavioral health and many others.
When I spoke with Pikaart, she had words of warning for the Cortez community: “When corporations or someone even threatens to close a labor and delivery unit, they inflict a wound on the entire hospital. And I think that that wound has been inflicted in Cortez.”
* * *
Al Huckins moved to Montezuma County a little over a decade ago, drawn to nonprofit work and the outdoor opportunities at the confluence of the mountains and the desert. Starting a family and maternal health care access were not priorities. When friends who lived in bigger towns and cities described their birth experience in a large hospital, it sounded big and impersonal, so when Huckins found out she was pregnant with her first daughter, initially she was expecting the same.

Al Huckins, photographed on June 15, 2023. Weeks before giving birth to her second child, Huckins was informed she would have to find another provider and location for the delivery, due to the closure of Southwest’s birthing center; the directive was eventually rescinded. Photo by Corey Robinson / Special to The Colorado Trust
But after meeting with her OB-GYN at the Southwest birthing center, Huckins felt the opposite. Complications during her delivery resulted in a five-day stay at Southwest in 2021, which only reinforced Huckins’ positive impressions. The providers cared. Her recovery and the health of both her and her newborn daughter seemed personal to them.
“I remember thinking, ‘I don’t know that I want to leave,’” she said, referring to the excellent care she felt she received at the birthing center.
Schmitt and Kaplan learned about the decision to close the birthing center on June 7 when the then-interim CEO David Faulkner called them into his office the day before he was set to publicly announce the closure. “His argument was because it’s such a costly unit and it doesn’t bring in the hospital any money,” Schmitt recalled. Schmitt was about to take a leave of absence for a family medical emergency, leaving Kaplan, who was eight months pregnant, on the hook for arranging the transition of care for roughly 80 patients in less than two weeks.
According to Schmitt and Kaplan, no one discussed the hospital’s reported financial difficulties and the birthing center’s potential closure with them beforehand. “There was no discussion of any cost-saving measures or streamlining the clinic or making things more productive so that we could save money,” Schmitt said.
Schmitt wondered what they were going to do about the dozens of patients who had established care at the hospital and were set to give birth within the coming six weeks. “There was no plan whatsoever,” Schmitt told me.
One of them was Huckins, whose due date for her second child was the day before the birthing center was supposed to close. The sudden change of plans made Huckins anxious because of the complications with her last delivery.
“I was pretty nervous to switch care that late into my pregnancy,” she said. At Southwest, the physicians and nurses knew her and had helped deliver her first daughter, which made Huckins feel safe. Now, she was getting a letter saying she’d have to switch to another doctor just weeks before she was due.
As soon as Schmitt and Kaplan learned of the decision to close the birthing center, they began strategizing how to fight back. Schmitt reached out to community members, who organized a Facebook group called Save the Hospital. The following day, after Southwest Health System made its public announcement about the center’s closure, they held a rally in front of the hospital. More than 50 people showed up, many holding signs that read “Keep our babies local” and “Care close to home, unless you are a woman.”
Another citizen group formed called Friends of the Hospital and reached out to other local stakeholders who would be affected by the center’s closure: emergency room physicians who would now be tasked with delivering babies, and EMT personnel who would have to deal with potentially life-threatening pregnancy or birth complications. The group arranged an open meeting with the health system board to share their concerns, with one ambulance driver saying what a disaster the closure would be for the county’s emergency services.
All the community mobilizing worked. On June 19, Southwest announced the birthing center would remain open after all. Yet the hospital reported laying off nine people to cut costs elsewhere.
Community Hospital Corporation Senior Vice President Joe Thomason apologized at a Montezuma County Hospital District board meeting on June 14 for how the birthing center closure was handled and acknowledged that the communication, preparation and process in which the closure played out was done poorly. According to meeting minutes, he added that the hospital is not in danger of closing, but that many small hospitals are having to make hard decisions related to deliveries as this service requires significant resources to be done safely and correctly. (The hospital district is in charge of levying taxes that pay for the physical hospital plant and infrastructure, but Southwest is the entity that manages hospital operations.)
Shirley Jones, the chair of the Southwest Health System board, later elaborated on the financial and operational challenges facing the birthing center, including the need for locum physicians that can cost the health system upwards of $5,000 per day. Though the birthing center remains open, Jones advised that unless the hospital can recruit more permanent physicians to cover calls and other adjustments, “it will remain financially unfeasible to keep the department open,” according to the meeting minutes, noting that many other critical access hospitals do not provide such services.
In Southwest’s written statement for this story, it noted that since the beginning of August 2023, the hospital has had roughly 30 providers interested in coming to work at Southwest Memorial and as of September they have completed 10 onsite interviews, with a few more to schedule in the coming months. The hospital has extended an offer to three providers and is actively discussing with others the possibility of working at Southwest in the future.
For Schmitt, the reversal has brought only temporary relief. Many patients had already started the process of transitioning their care to Durango, so the new decision left them in limbo, without knowing who and what to believe. Schmitt noted the irony that improving the image and the quality of care at the hospital was the reason she was hired six years ago.
“Our community is losing confidence in the hospital,” she said. “In my opinion, they’ve just totally undone everything that I’ve been doing since 2017.”
In late August, Kaplan gave birth to her son at the Southwest birthing center, with Schmitt attending to the delivery. Surrounded by nurses Kaplan knew and in her own small community, Kaplan felt like she was part of a family. It was the kind of personalized care that had made such a big impression on her when she started working at Southwest Memorial Hospital.
“I think that’s a huge part of what makes this place special,” she said.